iCAN

Cancer therapies, what’s the difference
Cancer care is a rapidly developing field, and there is a range of evidence-based treatments to suit the needs of all individuals.
Conventional medicine attempts to pinpoint, control and treat cancer as quickly and effectively as possible. However, there is now also a growing field of integrative oncology, incorporating complementary therapies which pay attention to the person as a whole, not just the cancer.
What are my options? What’s on offer?
When you’re facing a cancer diagnosis, terms like ‘conventional’, ‘complementary’, or even ‘alternative’ therapy can be confusing and overwhelming. This uncertainty around terminology and treatments can often lead to anxiety for patients, as well as health practitioners.
Following is a list of definitions to help you understand some of these terms.
Conventional therapies
Cancer Council Australia defines conventional therapies as those used to control or treat cancer and its symptoms by slowing or stopping the growth and spread of the disease.
Based on scientific evidence and clinical trials, conventional medicine includes surgery, radiation therapy (or radiotherapy) along with systemic treatments such as chemotherapy, hormone therapy, targeted therapy, immunotherapy and more.
Following are details on the most common conventional therapies.
Surgery
Surgery is a procedure in which the surgeon removes cancer cells from your body.
Radiation
Radiation therapy is a type of cancer treatment that uses high doses of radiation to kill cancer cells and shrink tumors.
Chemotherapy
A type of treatment that uses drugs to destroy cells in your body. It can be used before surgery or radiation for some cancers.
Immunotherapy
A process that helps your immune system work towards finding and destroying any type of abnormal cells or tumor growths within your body.
Targeted therapy
A type of cancer treatment that uses targeting agents to block certain proteins or pathways involved in the growth and survival of cancer cells. This slows down how quickly the cell growth occurs as well as make them more sensitive to radiation or chemotherapy treatments.
Hormone therapy
A treatment that slows or stops the growth of breast and prostate cancers by reducing levels of estrogen, testosterone, dehydroepiandrosterone sulfate (DHEAS) in order to arrest the growth of cancerous cells.
Stem cell transplant
A procedure that restores blood-forming stem cells in cancer patients who’ve had theirs destroyed by chemotherapy or radiation therapy.
Biomarker testing
By looking for biochemical indicators, like DNA and protein strands that are created in the body by cancer cells, biomarkers can help you or your doctor choose which treatment will work best with an individual’s needs and type of cancer.
COSA is the peak national body in Australia, representing health professionals who care for cancer patients. According to COSA, their mission is to develop and maintain high-quality clinical care of cancer patients in Australia.
Their definition of conventional medicine is treatments practised by those with a medical degree and by qualified health professionals such as pharmacists, physiotherapists, psychologists, social workers and registered nurses.
Complementary therapies
COSA defines complementary therapies as medicine and therapies that aren’t part of conventional treatment. They can, however, be used alongside conventional medicine to improve health.
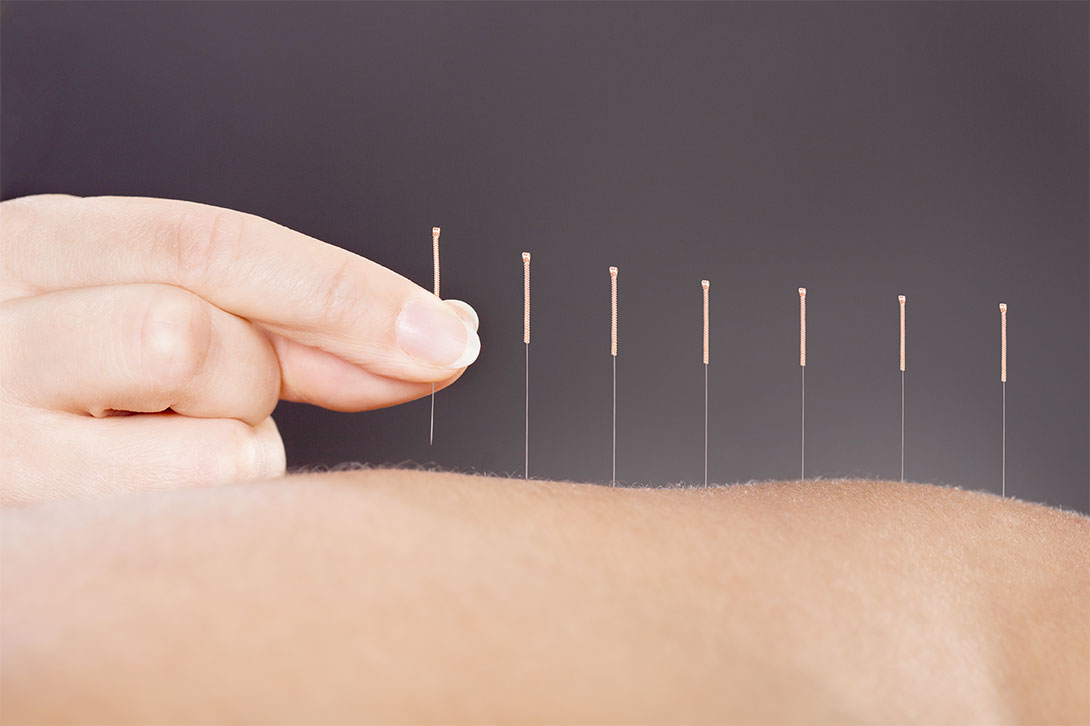
Complementary therapy covers a range of different healing techniques, disciplines and treatments. It includes ‘body-based’ practices such as acupuncture, massage and exercise. It also encompasses ‘mind-body’ techniques such as yoga, mindfulness and nutrition. Some Western and Chinese herbal medicines may also be classified as complementary.
Both COSA and the Cancer Council Australia support the use of some of the complementary therapies that have anecdotally shown to be safe and effective for people with cancer. It is important to note that although there are benefits, no complementary health product or practice is a proven cure for cancer.
Integrative medicine or integrative oncology
COSA refers to integrative medicine as the ‘blending’ of conventional and complementary medicine with the aim of using the most appropriate, safe and evidence-based care that is available.
Dr Judith Lacey is head of supportive care and integrative oncology at the Chris O’Brien Lifehouse hospital. She advocates for the concept of an ‘expanded toolbox’ of complementary medicine. She says that patients can access this toolbox to help manage their disease and symptoms to improve their quality of life.
“All of these interventions should be used together with traditional medicine or conventional cancer care,” Dr Lacey advises.
“The idea is to optimise health and improve quality of life and well-being but also to help the patient recover from treatment.”
When it comes to cancer care, Dr Lacey said the approach (known as integrative oncology) combines conventional and complementary therapies all in one big package.
“It’s all about looking at what happens to people during the cancer experience,” Dr Lacey says.
Some complementary therapies are able to improve specific symptoms such as fatigue, peripheral neuropathy and nausea, Dr Lacey explains. By combining and interacting with conventional treatments, they can also have a significant impact on a person’s well-being.
Some cancer and wellness centres are starting to adopt integrative oncology.
Dr Lacey encourages people to always speak to their oncologist about the complementary therapies that are available to them during their treatment.
Alternative therapies
Although the terms ‘complementary’ and ‘alternative’ are often used interchangeably, they are in fact, very different.
The Cancer Council defines alternative therapies and medicines as those used in place of conventional treatments and medicines, not alongside them, hence the word ‘alternative’.
“This is a different field entirely, where in place of conventional therapy, you’re offering an alternative,” Dr Lacey says.
According to the Cancer Council, there has been no scientific testing of many alternative therapies and so no proof they stop cancer growing or spreading. It also says that once tested, some therapies have proven to be ineffective.
“While side effects of alternative treatments are not always known, some are serious and can delay or stop the cancer being treated effectively,” the Council explains.
Cancer Council Australia urges people to be wary when considering using an alternative therapy or medicine. If your alternative practitioner is not registered with a governing body or professional association or has no accreditation, then these are warning signs.
Above all, patients should steer clear of any practitioner who asks them not to mention their alternative therapy to a treating doctor and specialist. If anyone says that they can cure cancer, be aware they are taking advantage of those in a vulnerable and desperate position.
Alternative therapies, however, cannot take the place of years of research and hard work that various medical practitioners have devoted their lives to.
If you are considering an alternative therapy, discuss it thoroughly with your oncologist, cancer care nurse, care team or someone qualified to assess your condition.
Resources
Further Reading
- Read Cancer Australia’s position on complementary and alternative therapies.
- Read Breast Cancer Network Australia’s position on complementary and alternative therapies
- See more on conventional cancer therapies at the Cancer Council
- Discover more on integrative treatment at the Australasian Integrative Medicine Association
- MacMillan Cancer Support on boosting physical or emotional health with complementary therapies
Research
Specialists
- Read more on Dr Judith Lacey.
Podcasts
- Listen to the integrative oncology podcast series from Dr Santosh of MD Anderson
- You Me & The Big C podcast episode The Alternatives gets to the facts on alternatives therapies
Webinars
- Register for the on-demand BCNA complementary therapies for breast cancer webcast
YouTube
- Watch interview with Dr Judith Lacey from LifeHouse on integrative oncology
We would love to know any resources you found helpful which we can share to help others. Please get in contact.