iCANThrive
Helping improve your emotional, social and mental wellbeing

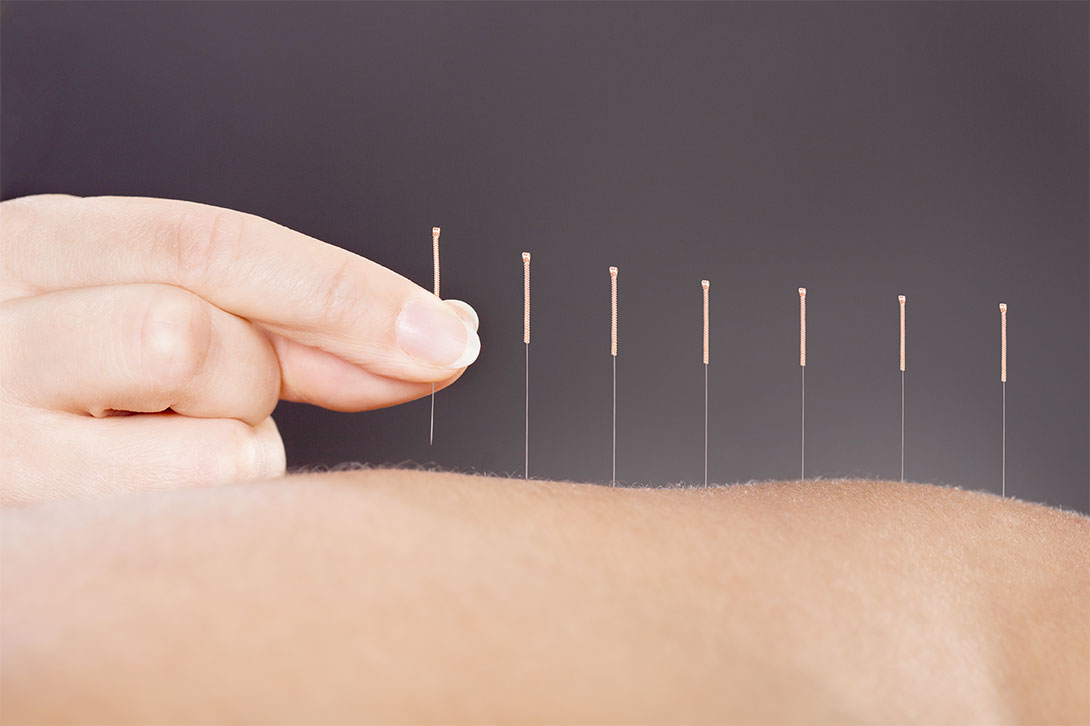
The hot flush; a guide on what to expect
For some females under ‘a certain age’, the collision of chemotherapy treatment and sudden menopause can be a severe shock, and a lot to take in. While undergoing chemotherapy oestrogen production is blocked, and this means that menopause comes way earlier than expected. This early visitor is also known as medical menopause, fake menopause or the super menopause, but it’s menopause just the same.
Professor Rod Baber is an obstetrician and gynecologist at the Royal North Shore Hospital, Sydney. After setting up a menopause clinic in the late 1980’s Rod noticed he was increasingly seeing post-treatment patients with menopausal symptoms.
Sleepless in Sydney
Prof Baber says it is when treatment finishes that menopausal symptoms usually begin, and these can go on for several months.
“Many of the cancer chemotherapy drugs will cause damage to the ovaries and destroy follicles,” he explains.
“The oestrogen deficiency induced by chemo or surgery produces menopausal symptoms that can be quite severe. Women tell us that their sleep is disrupted, they can have insomnia, along with frequent hot flushes which can come on suddenly, occur frequently, and compromise and upset the patient considerably.”
He adds that the full range of symptoms includes hot flushes, night sweats (hot flushes that happen at night), a red face, poor memory, mood changes, poor sleep, loss of concentration, muscle and joint aches and pains, depression and sudden fleeting aggression.
Not in the mood?
As time goes by, women can suffer from a dry vagina. Oestrogen provides lubrication and elasticity to the vagina. When the vagina becomes dry, it also loses elasticity, which means that intercourse can be difficult and painful. Even if you are not having intercourse, a dry vagina can be painful. There are over-the-counter remedies and treatments to help ease the problem.
Prof Baber advises that treating menopause is all about managing it. He suggests you avoid things that may trigger hot flushes, like alcohol, coffee and spicy foods. Another tip is to dress in layers so you can take something off if it gets hot.
“Cognitive behavioural therapy can help one learn to deal with hot flushes. There are also pharmaceutical blood pressure drugs like Clonidine, drugs for nerve pain, and various antidepressants, which taken in low doses, can offset the flushes with few side-effects,” he says.
Luan’s story
Luan, 48, was diagnosed in 2017 with pleomorphic invasive lobular breast cancer. She went into medical menopause after her second chemotherapy. For some, this would have been concerning but for Luan, it had a hidden advantage, in that her cancer was what is termed ‘oestrogen-positive’. This means that oestrogen assists in advancing the cancer.
“For me, it was a good thing to have medical menopause because I didn’t want to produce oestrogen which would ‘feed’ the type of cancer I had,” Luan explains.
After finishing chemo in 2018, Luan had a skin-sparing mastectomy. This is a technique that preserves as much of the breast skin as possible. She then followed up with radiotherapy, after which she started Tamoxifen, a hormone-blocking treatment. The blocker stops the cancer cell receptors from taking in any oestrogen and then multiplying.
“After a year my oncologist put me on an aromatase inhibitor (AI) to ease or stop oestrogen production. The reason for this is because even though you can be in menopause, your body produces oestrogen in different ways. One of which is the conversion of fat cells, which I did not want to happen. The AI stops this from happening. I was only on that for eight weeks though as I got a period after six weeks. I’m now back on Tamoxifen, which means the menopausal symptoms are normal and not as drastic as when I was taking an AI,” she notes.
Like those that Prof Baber describes, Luan’s symptoms include hot flushes, night sweats and ‘memory fog’, but she goes on to say that there is a lot more to it.
“Menopause is more than hot flushes and getting sweaty. My symptoms, which I’m still struggling with, are fatigue, ‘memory fog’ and struggling with my vocabulary at times. I get hot flushes day and night sweats, 80 per cent of which are preceded by an anxiety attack, like a dread, which starts in my stomach. It’s like a jolt, which wakes me up in the middle of the night,” she details.
‘There’s also the coldness that comes after the flush. In menopause the temperature range decreases, so I get hotter at lower temperatures and colder at higher temperatures. I’ll have a hot flush at night and fling the blankets off and then because I feel cold, I’ll start freezing and have to put the blankets back on.”
She says it took her a while to identify the ‘memory fog’ as menopausal as it’s also associated with the chemotherapy side effect ‘brain fog’, ‘chemo fog’ or ‘cancer fog’.
Be pro-active
What Luan strongly recommends is to soak up all the information on offer by the experts, and to push them on it.
“I was told my periods would most likely stop during chemotherapy but information about other menopause symptoms didn’t come from my oncologist at the time. What worked for me was attending the Early Breast Cancer group held at the Mater hospital in North Sydney. It’s a six-week program for women going through treatment at whatever stage, and each week focuses on different topics like oncology, surgery, diet, exercise and menopause. I really like the evidence-based studies that come from the experts. I also found reaching out to communities online like Instagram helped me connect with others. The Breast Cancer Network Australia also has great resources including chat forums where people can share,” Luan says.
“More importantly, as my current oncologist said, you need to acknowledge that you’ve had two life events: one is cancer and one is menopause, and to recognise the significance of them as being massive life events. This was really profound for me.”
‘‘Chemo is likely to bring on an early menopause. But don’t give up. There are doctors interested in helping you make your way through. Most women come out having good lives, and we can usually find things to help them alleviate their symptoms.” Prof Baber adds.
Resources
Products
- For a Dry Vagina try a silicone-based moisturiser such as, Replens.
Organisations
- OCA factsheet on cancer treatment and early menopause.
- BCNA factsheet on menopause and cancer.
- The Australian Menopause Society on dealing with early menopause.
- The Menopause Charity.
- The International Menopause Society.
Specialists
- Read more on Dr Rodney Baber.
Social media
- Follow Luan’s story on Instagram @unwritten.me.
- @thetittygritty talks Menopause after cancer.
- @breastcancernow chats with @oriordanliz on dealing with the side effects of hormone therapy.
- Other Instagram accounts @dee_before_c , @big_rozzys_advantures.
Books
- Dr Nicola Gates, The Feel Good Guide to Menopause.
We would love to know any resources you found helpful which we can share to help others. Please get in contact.